Atrial fibrillation or AF is the most common heart rhythm disorder and is defined by its irregular and often accelerated heart beat. Untreated atrial fibrillation increases the chance for certain serious disorders like stroke, heart failure, diabetes, dementia and hypertension. Getting diagnosed and treated in time is therefore of vital importance.
The heart and the heart rhythm
The heart is a hollow muscle that provides our tissues and organs with oxygen. The heart accomplishes this task by contracting and pumping blood throughout our body. The heart of a healthy adult contracts around 60 to 100 times a minute in a regular rhythm.
These contractions are triggered by electrical impulses. The electrical signal starts in a group of cells at the upper portion of the right atrium, called the sinus node. The sinus node sends out an electrical impulse which causes the atria or heart chambers to contract. Next, the electrical impulse travels to the area that connects the atria with the ventricles, the atrioventricular node. As the signal continues to the ventricles, they also contract.
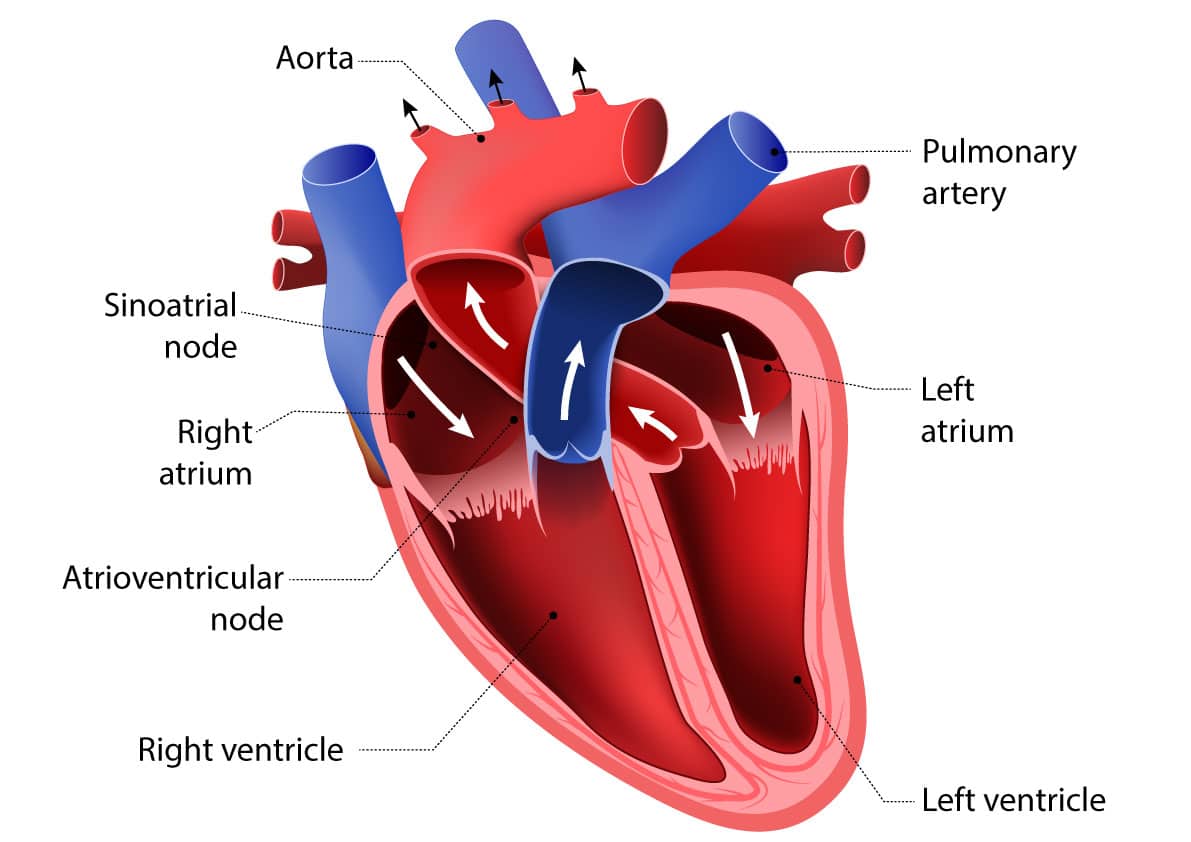
The anatomy of the heart.
What is atrial fibrillation?
Atrial fibrillation or AF is a heart rhythm disorder that causes the heart to beat in an irregular and often accelerated manner. The cause is a malfunction in the electrical system of the heart, where all electrical impulses normally are fired in a regular way by the sinus node. In AF patients the electrical signals start from different places in the heart, resulting in a chaos of electrical impulses. This chaotic electrical activity causes the chambers of the heart to contract irregular and less powerful, they fibrillate or quiver, hence the name atrial fibrillation. AF can cause the atria to quiver up to 400 times per minute. During an atrial fibrillation episode your heart rate can go up until 150-200 (irregular) beats per minute when at rest.
Atrial fibrillation is one of the most common heart rhythm disorders. The more we age, the higher the risk of atrial fibrillation. From the age of 40, one has a 1 in 4 chance to develop AF over their lifespan, the risk increases the most after the age of 65.
An important characteristic of AF is that it can come and go. Some patients have episodes that last a few minutes to a few hours and then disappear again. Others have episodes a few times a year, some have it permanently. The fickle character of AF makes it difficult to get a correct diagnosis.
Different types of Atrial fibrillation
Atrial fibrillation (AF) can present in a few different variants:
- Paroxysmal atrial fibrillation: Episodes come and go and can occur without any symptoms. Episodes can last anywhere between a few minutes up to a week.
- Persistent atrial fibrillation: When someone suffers from this type of atrial fibrillation their heart rhythm does not return back to normal by itself (episodes last for at least a week). A medical intervention (electroshock or medication) is needed to normalise your heart rhythm and/or to make any symptoms go away.
- Permanent atrial fibrillation: For this type of AF, your doctor already tried to normalise your heart rhythm, but did not succeed to do so. You then suffer from a lasting heart rhythm disorder. If symptoms occur they will be treated, but the rhythm disorder itself is ‘accepted’ in this case.
If untreated, patients can progress through these phases. Where you might initially only suffer from AF a few minutes every few months, AF can become a persistent problem over time.
Symptoms
About 40% of atrial fibrillation (AF) patients will never feel any symptoms and are therefore most of the time unaware they suffer from the disease. So patients often only get a diagnosis, when doctors are looking for the cause of complications that occurred (e.g. AF is found as the cause of a stroke)

When you do experience symptoms, these are the most common ones:
- Palpitations: which feel as a rapid fluttering in the chest, a pounding sensation in the chest , or a flip-flopping in the chest.
- General fatigue and weakness
- Reduced exercise capacity
- Dizziness or lightheadedness
- Confusion
- Shortness of breath
- Chest pain
Risk factors:
Certain factors can increase the risk of atrial fibrillation (AF). Some of these factors are:
- Age: The older you get, the higher the risk of AF.
- Other heart conditions: Individuals suffering from heart valve issues, congenital heart disease, congestive heart failure, coronary artery problems, history of heart attacks or heart surgery have an increased risk of AF.
- High blood pressure: Elevated blood pressure, certainly when ill-managed, increases the risk of AF.
- Other chronic diseases: individuals with specific chronic diseases like thyroid problems, sleep apnea, metabolic syndrome, diabetes, chronic kidney disease or lung disease have an increased risk of AF.
- Alcohol: alcohol can induce AF episodes.
- Obesity: individuals with obesity have an increased risk of developing AF.
- Family history: An increased risk for AF runs in some families.
What makes atrial fibrillation so dangerous?
During an atrial fibrillation (AF) episode, the upper chambers of the heart quiver or fibrillate up to 400 times per minute. This impairs the normal pumping function of the heart significantly. The impaired pumping function results in a stagnation of blood in the heart, which in its turn increases the chance of forming blood clots. Blood that is not moving, starts to coagulate quickly. These blood clots can end up in your bloodstream where they get stuck when vessels become too small for the particular clot. A blood clot that gets stuck in the body is called an embolism.
When a blood clot makes it to the brain and gets stuck in the blood vessels of the brain it cutts of that part of the brain from oxygen supply. This is what we call a stroke or cerebrovascular accident. This is the most feared complication of AF, since a stroke can be life threatening and can lead to paralysis and/or loss of speech.
Diagnosis and treatment
Luckily it doesn’t need to get to that. If detected early and treated correctly, atrial fibrillation (AF) induced strokes can be prevented.
Diagnosis:
Diagnosing atrial fibrillation can be done through an electrocardiogram or ECG or through a PPG measurement (the technique used by FibriCheck). Performing an ECG requires some medical background, a PPG measurement on the other hand is easy and can be done by anyone of us at home.
However diagnosing atrial fibrillation can be quite challenging. Atrial fibrillation episodes come and go and are therefore often missed during a doctor’s consult. The reason is that when the patient is lying on the examination table, his or her heart rhythm can be perfectly normal, but unfortunately this is only a snapshot. At home solutions like FibriCheck (using the PPG technique) increase the chance of a quick diagnosis significantly as patients can check themselves everyday and/or when experiencing symptoms.
Treatment:
The treatment of atrial fibrillation consists of several aspects:
- Rate control: Rate control focuses on slowing down the elevated heart rate.
- Rhythm control: If patients still experience symptoms when their heart rate is under control, doctors will try to normalize the heart rhythm.
- Stroke prevention: Preventing the formation of blood clots in the heart.
- Treating comorbidities: Treating other medical conditions that cause or aggravate atrial fibrillation.
Rate control
Rate control focuses on slowing down an elevated heart rate, which makes the pumping function of the heart more efficient. After which the symptoms of the patient will diminish or disappear.
Rate control can be done with the help of medication such as beta-blockers, calcium channel blockers or digoxin. If the heart rhythm cannot be normalized for a patient, frequency control is the primary goal of the treatment.
Rhythm control
The purpose of rhythm control is to try to restore and then maintain a normal, regular heart rhythm. Restoring the normal sinus rhythm is called cardioversion. This can be done by administering medication (anti-arrhythmics) or by administering an electrical shock. However, the chance of a successful cardioversion is difficult to predict and is greatest in young patients, when AF is not yet present for a long time (hours to a few days) and if there are no other heart problems.
To maintain a normal heart rhythm after successful cardioversion, patients are often prescribed maintenance treatment with “antiarrhythmic drugs”.
If the cardioversion fails or atrial fibrillation episodes continue to return regularly, the cardiologist can propose an ablation. With this surgical technique the doctor blocks the electrical stimuli that cause the irregular heart rhythm. This is done by burning or freezing the part of the heart where the disturbed stimuli are generated or pass through. The scar tissue that is formed, blocks the conduction of the electrical stimuli.
Stroke prevention
To minimize the formation of emboli and the risk of strokes, anticoagulants can be prescribed. Anticoagulants dilute the blood and minimize the chance that blood clots are formed. But they also increase the risk of bleeding. Doctors must therefore carefully outweigh the risks and benefits for each individual patient before prescribing anticoagulants.
Tackling comorbidities
A healthy lifestyle is important in the treatment of atrial fibrillation (AF). Other underlying problems, probable causes of AF and risk factors in the development and maintenance of AF must be addressed.
How to do that?
- Control and treat high blood pressure (hypertension);
- Control and treat diabetes;
- Strive for a healthy weight;
- Quit smoking;
- Limit the consumption of alcohol, caffeine and other stimulants;
- Tackle underlying problems such as other heart conditions, lung diseases, chronic renal failure, thyroid problems, sleep apnea, infections …;
- Ensure enough physical activity such as walking. Note: intensive endurance sports (grubbing, running, cycling, etc.) can lead to arrhythmias;
- Correctly follow the prescribed medication scheme.
FibriCheck: monitor your heart rhythm through your fingertip
Created on August 14th, 2019 at 12:47 pm
Last updated on June 27th, 2024 at 09:12 am




